HIGHLIGHTS
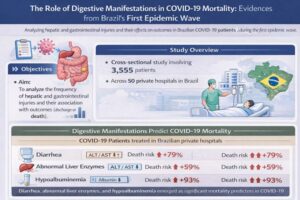
- To analyze the frequency of hepatic and gastrointestinal injuries and their association with outcomes (discharge or death).
- Cross-sectional study involving 3555 patients across 50 private hospitals in Brazil.
- Diarrhea, abnormal liver enzymes, and hypoalbuminemia emerged as significant mortality predictors in COVID-19 patients treated at Brazilian private hospitals.
ABSTRACT
Background –
COVID-19, caused by SARS-CoV-2, is primarily characterized by respiratory symptoms but also significantly affects the gastrointestinal (GI) tract and liver. Emerging evidence suggests that GI and hepatic manifestations may influence disease severity and outcomes. In Brazil, where disparities between public and private healthcare systems are pronounced, understanding these associations is crucial for optimizing patient management. This study aimed to evaluate the frequency and prognostic implications of digestive and hepatic injuries in hospitalized COVID-19 patients. Objective – To analyze the frequency of hepatic and gastrointestinal injuries and their association with outcomes (discharge or death). Methods – A retrospective cross-sectional study analyzed 3,555 patients from 50 private hospitals in Brazil (March–December 2020). Inclusion criteria were age ≥18 years, RT-PCRconfirmed COVID-19, and written consent. Demographic data, comorbidities, GI symptoms (diarrhea, nausea/vomiting, abdominal pain), liver enzymes (ALT, AST), and outcomes (discharge, mortality, ICU admission) were collected via REDCap. Statistical analyses included logistic regression to identify mortality predictors. Results – Among 3,555 patients (59.9% male, mean age 55.8 years). A total of 42.2% of patients presented with at least one gastrointestinal (GI) symptom at admission. Diarrhea was reported in 15%, nausea or vomiting in 13.6%, and abdominal pain in 6.5%, with symptom overlap among patients. The deceased group exhibited significantly higher alanine aminotransferase (ALT) (P=0.019) and aspartate aminotransferase (AST) (P=0.026) levels, representing 4.2- and 8.4-fold increases, respectively, with a higher AST/ALT ratio in fatal cases (1.69 vs 0.84). COVID-19 patients in Brazilian private hospitals showed hepatic abnormalities (AST 354.1 IU/L vs 42.1 IU/L in deceased vs discharged patients, P=0.026), with diarrhea associated with lower mortality (OR 0.61; 95%CI 0.42–0.88), while chronic liver disease (OR 2.95; 95%CI 1.35–6.41) and hypoalbuminemia (OR 0.22; 95%CI 0.11–0.38) emerged as independent predictors of death. Conclusion – Hepatic abnormalities and gastrointestinal symptoms are important markers of COVID-19 severity. Diarrhea, liver enzyme alterations, and serum albumin levels were significant predictors of mortality. Future strategies should prioritize hepatic monitoring, nutritional support, and healthcare equity through targeted interventions for high-risk groups, particularly in resource-limited settings.
AUTORES
Elvis Paim FERREIRA, Mariana da Silva ARBUÉS, André Castro LYRA and Lourianne Nascimento CAVALCANTE