HIGHLIGHTS
- This retrospective, multicenter study evaluated the accuracy of six predictive models of death within 90 days in 461 patients hospitalized for decompensated cirrhosis.
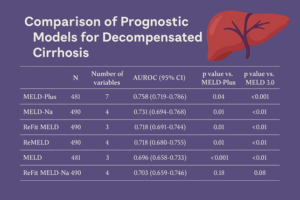
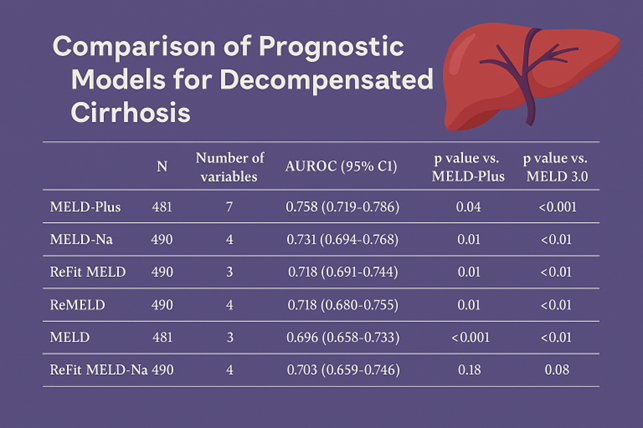
- The scores presented an area under the receiver operating characteristic curve of 0.703–0.758, indicating a good ability to discriminate between survivors and deceased patients during the considered period.
- The comparison between the models did not unequivocally establish the superiority of one model over the other.
ABSTRACT
Background – The natural history of cirrhosis is characterized by an asymptomatic phase (compensated cirrhosis) followed by a rapidly progressive phase (decompensated cirrhosis). The ability to predict the survival of patients with cirrhosis is crucial for decision-making, some as complex as the indication for a liver transplant. Several models have been developed and validated. Objective – To analyze and compare the performance of models in predicting 90-day mortality among patients hospitalized with decompensated cirrhosis. Methods – A sample of 481 hospitalized patients, with a mean age of 59.04 years 73% male, diagnosed with decompensated cirrhosis and a mean Child-Pugh score of 9. The prognostic models were calculated based on tests performed on admission: MELD-Na, MELD-Plus, MELD 3.0, ReMELD, Refit MELD, and Refit MELDNa. The accuracy of the models was assessed by calculating the area under the receiver operating characteristic (AUROC) curve, and their respective 95% confidence intervals. Comparisons between the areas were conducted using the DeLong test. A comparison was conducted among all scores, with a primary focus on MELD 3.0 and MELD-Plus. These specific scores were the focal points of interest. Results – The scores presented AUROC curve values of 0.703–0.758, indicating a moderate capacity to discriminate between survivors and deceased patients during the considered period. The comparison between the models did not unequivocally establish the superiority of one model over the other. Conclusion – The scores have a limited predictive ability for death within 90 days in patients with decompensated cirrhosis. Our study is unable to establish the prognostic superiority of a specific scoring system. Keywords – Liver cirrhosis; mortality; end stage liver disease; clinical decision rules.
AUTORES
Ajácio Bandeira de Mello BRANDÃO1, Isadora Zanotelli BOMBASSARO1, Gabriela Perdomo CORAL1,2, Jonathan SOLDERA3,4 and Carlos KUPSKI5