- HIGHLIGHTS
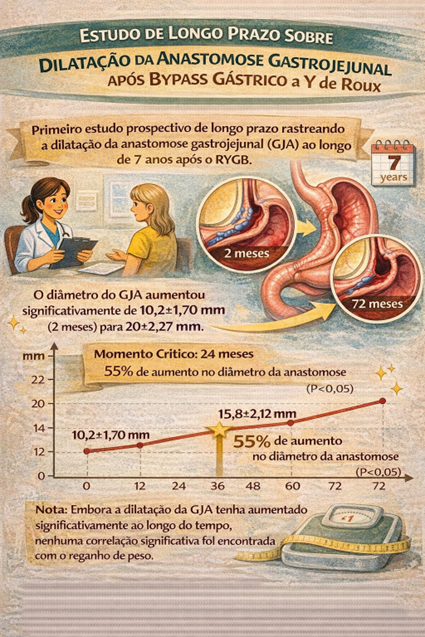
- First long-term prospective study tracking gastrojejunal anastomosis (GJA) dilation over 7 years post-RYGB.
- GJA diameter increased significantly from 10.2±1.70 mm (2 months) to 20±2.27 mm (72 months).
- Critical timepoint: 24 months post-surgery marked a 55% enlargement in anastomosis diameter (P<0.05).
Although GJA dilation increased significantly over time, no significant correlation was found with weight regain.
ABSTRACT
Background –
Obesity is considered a global epidemic and has shown a progressive increase in recent decades. Bariatric surgery, such as Roux-en-Y gastric bypass (RYGB), is the most effective sustainable weight loss option. However, weight regain is one of the challenges facing patients and is attributed to several factors, including dilatation of the gastrojejunal anastomosis (GJA). Objectives – The central objective of this study is to correlate the influence of time on GJA widening in patients undergoing RYGB over a 7-year period. Methods – Prospective and longitudinal study conducted over 7 years in patients undergoing RYGB. Surgical and endoscopic procedures were performed in a medium hospital in the same city. Weight, body mass index (BMI) and GJA size were assessed at intervals of 2, 6, 12, 24, 30, 48, 60, and 72 months after the surgical procedure. Results: The highest mean value in the distribution of anastomosis diameter was 20±2.27 mm at 72 months after surgery. The lowest mean value was 10.2±1.70 mm at 2 months after surgery. The analysis showed that there is a significant effect of time on anastomosis diameter, with statistically significant differences in the mean value between 2, 6, 12, 24, 60, and 72 months after surgery (F(1,724,5,172)=9.555, P<0.05). Conclusion – Multiple comparative analysis showed that there are statistically significant differences between the mean lengths of anastomosis across the times studied, with a greater influence of the time factor 24 months after surgery.
AUTORES
Gustavo Henrique Xavier Caseiro, Vitor Ottoboni Brunaldi, Maisa Buissa, Roberto Luiz Kaiser-Junior, Carolina Colombelli Pacca and Luiz Gustavo de Quadros