HIGHLIGHTS
- Recognize patients with extra pancreatic manifestation in autoimmune pancreatitis.
- It is a retrospective study that was done through revision of the patient clinical, laboratory and imaging including CT/MRI of the abdomen and chest CT of all patients.
- The extra pancreatic associated diseases in AIP candidates, were detected in 23 patients (76.6%).
- Type 1 AIP has been associated with several extra pancreatic manifestations determining different clinical outcomes
ABSTRACT
Background –
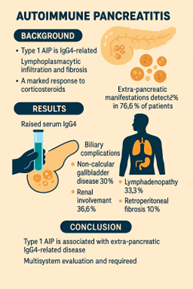
Autoimmune pancreatitis (AIP) is a specific form of pancreatitis that is characterized by obstructive jaundice and sometimes associated with pancreatic masses, lymphoplasmacytic infiltrate and fibrosis, with a marked response to steroids. According to International Consensus Diagnostic Criteria AIP is categorized into type 1, type 2, and not otherwise specified (NOS). AIP-1 is one of the presentations of the IgG4- related disease (IgG4-RD) characterized by lymphoplasmacytic infiltration and more than ten IgG4-positive plasma cells per high-power field (HPF), storiform fibrosis, and obliterative phlebitis. Clinically, IgG4-RD is a systemic disease that can affect all organs. It can affect the bile ducts, kidneys, lymph nodes, prostate, and retroperitoneum. Objective – Recognize patients with extra pancreatic manifestation in autoimmune pancreatitis as soon as possible to achieve optimal outcomes. Methods – A retrospective comparative study was conducted on the previously hospitalized patients to our main university hospital, during the period from June 2022 till June 2024. It is a retrospective study that was done through revision of the patient clinical, laboratory and imaging including CT/MRI of the abdomen and chest CT of all patients. 60 patients with pancreatitis were enrolled in the study. It was diagnosed based on at least two criteria of the following: (1) typical abdominal pain, (2) elevated amylase and/or lipase greater than 3 times, and (3) radiological findings match with pancreatitis. Cases were divided according to the International Consensus Diagnostic Criteria (ICDC) into group A: Autoimmune pancreatitis (AIP) defined by a specific form of pancreatitis characterized by obstructive jaundice with or without pancreatic masses, lymphoplasmacytic infiltrate and fibrosis (from laparotomy biopsies in suspected pancreatic cancer) and a marked response to steroids. And group B: conventional pancreatitis, with 30 patients in each group. Results – A raised serum IgG4 was found in group A patients ranging from 135.0 mg/dL to 212.0 mg/dL with >95% specificity and sensitivity for AIP. The extra pancreatic associated diseases in AIP candidates, were detected in 23 patients (76.6%). Biliary tree complications were seen at 22 patients (73.3%), non calcular gall bladder disease was detected in 9 patients (30%), renal complications were found in 11 patients (36.6%), irrelevant lymphadenopathy in 10 patients (33.3%), retroperitoneal 3 patients (10%). In group B: there were biliary obstructive in 9 patients (30%), calcular cholecystitis was found in 19 patients (63%), with no other recorded extra pancreatic diseases. Chi square and Fisher Exact tests revealed significant differences between the two groups, as regards the extra pancreatic diseases in association with group A. Conclusion – Type 1 AIP has been associated with several extra pancreatic manifestations determining different clinical outcomes. Therefore, patient monitoring and a multisystem evaluation approach are required.
AUTORES
Rania A M ABOUYOUSSEF, Mohamed Saied ABDELGAWAD, Mahmoud AGHA and Marwa IBRAHIM